Инфекции мочевыводящих путей (МВП) по частоте занимают второе место после острых респираторных инфекций, а среди них самыми частыми являются инфекции нижних отделов МВП – острый и рецидивирующий цистит. Этиологическим фактором острых респираторных инфекций, как правило, выступают вирусы, и в последние годы эксперты настоятельно не рекомендуют назначать антибиотики при нетяжелых инфекциях верхних дыхательных путей. В то же время инфекции нижних МВП преимущественно бактериальные и подразумевают обязательное назначение антибактериальной терапии. Таким образом, частота назначений антибиотиков в амбулаторной практике для лечения инфекций МВП не уступает, а может, и превышает частоту назначения антибиотиков при респираторных инфекциях, по крайней мере взрослым пациентам. Следовательно, правильное назначение антибиотиков при инфекциях МВП важно не только применительно к излечению конкретного пациента, но и в рамках всей медицины и общества с учетом современной стратегии сдерживания антибиотикорезистентности, что находит отражение в документах научных профессиональных обществ [1, 2], международных организаций [3, 4] и Правительства РФ [5].
Сложности правильного назначения антибиотиков при инфекциях нижних МВП объясняются тем, что пациенты приходят на прием не только к урологу, но и к врачу общей практики, терапевту, педиатру, гинекологу. Именно поэтому так важна гармонизация практических рекомендаций по лечению цистита в разных медицинских дисциплинах. Кроме того, значительное число женщин с симптомами острого цистита вообще не обращаются к врачу и, приобретая антибиотик в аптеке, получают совет у работника первого стола. В последние годы в России и за рубежом [2, 6–9] были опубликованы клинические рекомендации по инфекциям МВП. Во всех рекомендациях эксперты пришли к консенсусу по выбору антибиотиков для лечения цистита:
- антибиотики первой линии терапии: нитрофураны или фосфомицин трометамол;
- антибиотики второй линии терапии: пероральные цефалоспорины III поколения или амоксициллин/клавуланат;
- нерекомендуемые антибиотики: фторхинолоны, нефторированные фторхинолоны, ко-тримоксазол, незащищенные аминопенициллины.
Среди нитрофуранов в зарубежных рекомендациях приводится нитрофурантоин, в отечественных рекомендациях есть также фуразидин, который отсутствует в большинстве стран Европы и Америки. В свою очередь в зарубежных рекомендациях в числе препаратов первой линии упомянут пивмециллинам, который в нашей стране отсутствует.
Представляется важным обсудить, какие учетные факторы принимают во внимание эксперты, рекомендуя или не рекомендуя антибиотик для лечения наиболее частой инфекции МВП – острого и рецидивирующего цистита. Цистит относится к нетяжелым инфекциям, поэтому врачи иногда позволяют себе небольшое творчество и вольно подходят к трактовке рекомендаций, в отличие от более тяжелых инфекций с серьезным прогнозом, например пиелонефрита, сепсиса.
В отличие от пиелонефрита, который является тканевой инфекцией с частым развитием бактериемии, при цистите бактериальная инвазия ограничивается в основном слизистой оболочкой мочевого пузыря, поэтому создание высоких концентраций антибиотика в моче, а не в тканях служит основным фармакологическим условием применения препарата при этом заболевании. То есть те антибиотики, которые характеризуются преимущественно почечным путем выведения, отвечают этим условиям. Однако целью антимикробной терапии остается микроорганизм – возбудитель инфекции, поэтому для лечения цистита требуются антибиотики, проявляющие высокую природную активность в отношении наиболее актуальных возбудителей. Со временем микробы приобретают способность выживать в присутствии антибиотика, т.е. формировать антибиотикорезистентность. Таким образом, текущая ситуация с резистентностью основных возбудителей мочевых инфекциям считается третьим учетным фактором, который надо принимать во внимание, рекомендуя антибиотик. И наконец, новая концепция рациональной антимикробной терапии подразумевает учет экологической безопасности антибиотика – его способности вызывать нарушение биоценоза на микро- и макроэкологическом уровне, вызывать селекцию антибиотикорезистентных бактерий. Эту новую концепцию следует учитывать при назначении антибиотиков, так как в глобальном аспекте нашей стратегической целью является сдерживание антибиотикорезистентности. Перечисленные факторы учитывают эксперты при создании рекомендаций по лечению инфекций МВП для врачей разных специальностей.
Таким образом, для выбора антибиотика при цистите следует оценивать следующие факторы:
1. Фармакокинетика антибиотика – преимущественно почечная экскреция с созданием высоких концентраций активного антибиотика в моче.
2. Антимикробная характеристика антибиотика:
a. Природная активность в отношении наиболее актуальных возбудителей;
b. Уровень приобретенной устойчивости микробов к антибиотикам в конкретном регионе.
3. Экологическая безопасность антибактериальной терапии:
a. Воздействие на микробиоту ЖКТ и урогенитальных органов – т.н. коллатеральный, или параллельный, ущерб, существенно различающийся для разных антибиотиков;
b. Селекция под действием антибиотика полирезистентных бактерий.
1. Фармакокинетика антибиотика
Для некоторых классов антибиотиков характерна исключительно почечная экскреция, препараты не подвергаются метаболизму в печени и выводятся почками в неизмененном виде, поэтому в моче достигаются очень высокие концентрации, превышающие минимально подавляющую концентрацию (МПК) основных патогенов в десятки, а то и в сотни раз. К таким классам антибиотиков относятся аминогликозиды, гликопептилы и липопептиды, сульфаниламиды, триметоприм, нитрофураны и фосфомицины.
Наоборот, антибиотики макролиды, линкозамиды, оксазолидиноны, тетрациклины характеризуются в основном печеночной элиминацией с желчью или путем метаболизма до неактивных соединений, поэтому достижение терапевтических концентраций этих антибиотиков в моче проблематично и они, как правило, не рекомендуются для лечения инфекций МВП.
Для представителей β-лактамных антибиотиков и фторхинолонов характерны различия в фармакокинетике. Среди β-лактамов преимущественно почечной экскрецией обладают все пенициллины и карбапенемы, а также большинство цефалоспоринов, однако есть исключения. Печеночное выведение характерно для цефалоспорина III поколения цефоперазона, а среди пероральных цефалоспоринов – для цефдиторена, который, в отличие от цефиксима и цефтибутена, не создает терапевтических концентраций в моче.
Среди фторхинолонов преимущественно почечная экскреция характерна для ципрофлоксацина, левофлоксацина, норфлоксацина, офлоксацина. Пефлоксацин и моксифлоксацин выводятся преимущественно печенью, поэтому не применяются в лечении инфекций МВП.
Из антифунгальных препаратов терапевтические концентрации в моче достигаются при назначении флуконазола, другие азолы (вориконазол, кетоконазол) имеют внепочечный путь элиминации, как и эхинокандины.
2. Антимикробная характеристика антибиотика
А) природная активность в отношении наиболее актуальных возбудителей.
Под природной активностью антибиотика подразумевают спектр его антимикробного действия. Практически важно выделять не только сам факт активности в отношении возбудителя (чувствительный, умеренно чувствительный и резистентный), но и его природную выраженность (или силу воздействия), которая оценивается по величине МПК и соотносится с достижимыми концентрациями в очаге инфекции. В зависимости от этого выделяют сильную, умеренную и слабую природную активность, причем в отношении микробов, которые лишены каких-либо генов устойчивости, – так называемые дикие штаммы.
Инфекции МВП, как правило, являются моноинфекциями, т.е. в качестве этиологического фактора выступает только один микроорганизм. По данным большинства эпидемиологических исследований, ведущим возбудителем острого цистита является Escherichia coli. Доля E. coli в этиологии неосложненного цистита была очень высока (80–90%) в ранних исследованиях, проведенных до 2010 г. [10–12], в последующих исследованиях несколько снизилась [13, 14].
В многоцентровом международном исследовании ARESC [13] изучена этиология острого неосложненного цистита.
E. coli занимала доминирующую позицию (72,6%), значительно меньшее значение имели Klebsiella pneumoniae (4,6%), Proteus mirabilis (2,4%), Staphylococcus saprophyticus (3,6%), другие Enterobacterales и Enterococcus spp. (11,1%), другие стафилококки и страптококки (5,8%). Необходимо подчеркнуть, что существенное доминирование E. coli прослеживается в исследованиях, где изучали этиологию острого неосложненного цистита.
В проведенном в 2017 г. в России большом многоцентровом исследовании RESOURCE с охватом практически всех регионов страны изучена этиологическая структура инфекций МВП у 84 318 пациентов, от которых получено 41 510 изолятов уропатогенов, причем эти пациенты были как с неосложненными, так и с осложненными и рецидивирующими инфекциями [15]. Основным возбудителем также была
E. coli, но ее доля была ниже (49,1%), чем при неосложненных инфекциях. При осложненных и рецидивирующих инфекциях существенно выше роль K. pneumoniae (9,5%), Enterococcus faecalis (8,7%), Enterococcus spp. (6,9%), S. saprophyticus (6,1%); среди других возбудителей выявлены стрептококки группы В (4,6%), P. mirabilis (2,9%), S. aureus (1,2%).
Таким образом, следует учитывать определенные различия в этиологии острых и рецидивирующих инфекций МВП, неосложненных и осложненных:
Острый неосложненный цистит:
- Преимущественно E.coli
Осложненный или рецидивирующий цистит:
- E. coli+Klebsiella pneumoniae+/- Proteus mirabilis
- Enterococcus faecalis+/-Staphylococcus saprophyticus
- Грамположительные возбудители ≈ 20%.
Природная активность антибиотиков в отношении наиболее актуальных возбудителей цистита приведена в табл. 1.

В отношении основного возбудителя цистита E. coli все приведенные антибиотики обладают природной активностью, однако сила воздействия разная: наиболее высокая природная активность имеется у цефалоспоринов III поколения, фторхинолонов, нитрофуранов и фосфомицина трометамола; несколько ниже – у амоксициллина/клавуланат и цефалоспорина II поколения цефуроксима; у цефалоспоринов I поколения, в частности цефалексина, активность в отношении E. coli крайне слаба, что нужно учитывать, так как в некоторых зарубежных рекомендациях данных антибиотик позиционируется для профилактики [7, 8].
В отношении других грамотрицательных патогенов высокой активностью обладают только фторхинолоны, активность других антибиотиков ниже и существенно варьируется.
В отношении E. faecalis реальной активностью обладают только нитрофураны и аминопенициллины, частично активны фторхинолоны (левофлоксацин >ципрофлоксацин); другие антибиотики лишены природной антиэнтерококковой активности. Неоднозначный вопрос по антиэнтерококковой активности фосфомицина трометамола. В инструкции по медицинскому применению фосфомицина трометамола сказано о наличии такой активности, в наиболее известном справочнике The Sanford Guide [16] приводятся данные о слабой и вариабельной активности, не позволяющей рекомендовать антибиотик в монотерапии.
По данным базы данных Европейской организации EUCAST (European Committee on Antimicrobial Susceptibility Testing), регламентирующие правила которой рекомендованы для применения в лабораториях РФ, фосфомицин не обладает реальной активностью в отношении энтерококков [17]. Приведены распределения МПК нитрофурантоина и фосфомицина для «диких» штаммов E. faecalis и S. saprophyticus, выделенных во всех странах Европы и лишенных каких-либо механизмов устойчивости. Вертикальная линия отделяет чувствительную популяцию (слева от линии) от устойчивой (справа) в соответствии с пограничными критериями: для нитрофурантоина – 64, для фосфомицина – 8 мг/л. Видно, что если значения МПК нитрофурантоина практически для всех штаммов E. faecalis находятся в диапазоне чувствительности, то для фосфомицина все значения МПК выше 8 мг/л, т.е. находятся в диапазоне устойчивости. Сходное заключение можно сделать при анализе распределения МПК для S. saprophyticus, т.е. реальная антистафилококковая активность у фосфомицина трометамола отсутствует.
В отношении E. faecium нитрофурантоин является единственным антибиотиком из перечисленных, обладающим природной активностью; в отношении стафилококков наряду с нитрофурантоином также высокоактивны амоксициллин/клавуланат и цефалоспорины I–II поколений, ниже активность у фторхинолонов и ко-тримоксазола.
B) уровень приобретенной устойчивости микробов к антибиотикам в конкретном регионе.
Текущую ситуацию с региональной антибиотикорезистентностью уропатогенов следует учитывать при разработке рекомендаций по лечению. В табл. 2 приведены данные о резистентности грамотрицательных возбудителей инфекций МВП (неосложненные+осложненные, острые+рецидивирующие), полученные в самом крупном эпидемиологическом исследовании RESOURCE, недавно проведенном в России (84 318 анализов мочи, 41 510 штаммов уропатогенов) [15].
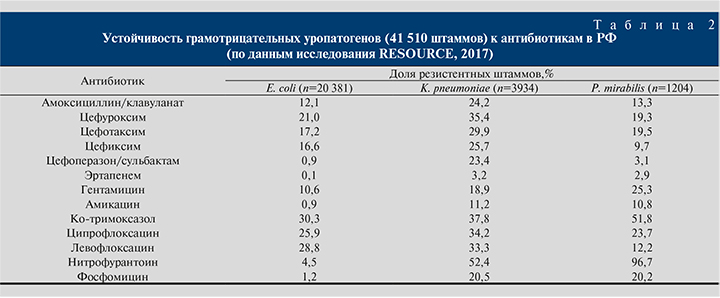
Для обсуждения этих результатов необходимо ввести понятие «эпидемиологический порог отсечения» (Epidemiological breakpoint), который используется для разграничения допустимого и высокого уровней устойчивости уропатогенов в популяции. В зарубежных и российских клинических рекомендациях для внебольничных уропатогенов используется порог отсечения 20% [2, 7, 9], подразумевающий, что антибиотик может быть рекомендован при устойчивости ниже 20% и ограничен в использовании при резистентности свыше порога отсечения.
В отношении самого частого возбудителя цистита E. coli устойчивость ниже порога отсечения наблюдается у нескольких пероральных антибиотиков – фосфомицина трометамола, нитрофурантоина, амоксициллин/клавуланата и цефиксима, а также парентеральных антибиотиков – амикацина, гентамицина, цефотаксима, цефоперазон/сульбактама. Последний антибиотик не применяется в лечении инфекций МВП из-за особенностей его фармакокинетики, но служит микробиологическим маркером чувствительности к другим ингибиторозащищенным цефалоспоринам (цефепим/сульбактам, цефотаксим/сульбактам), которые могут назначаться в стационаре для лечения госпитализированных пациентов.
Если в отношении E. coli есть несколько возможностей терапии, то против других грамотрицательных уропатогенов опции пероральной терапии в амбулаторной практике крайне лимитированы: в случае выявления K. pneumoniae можно назначать фосфомицина трометамол (устойчивость – 20,5%), P. mirabilis – цефиксима и фосфомицина трометамола. Таким образом, в случае осложненных и рецидивирующих инфекций МВП, вызванных K. pneumoniae, надежные опции пероральной терапии отсутствуют, а такой пациент, вероятно, должен быть госпитализирован для проведения парентеральной антибактериальной терапии карбапенемом или амикацином. Следует также отметить, что новые фторхинолоны (левофлоксацин) не имеют преимуществ в отношении грамотрицательных уропатогенов по сравнению с ципрофлоксацином, а цефалоспорин II поколения цефуроксим уступает цефалоспоринам III поколения.
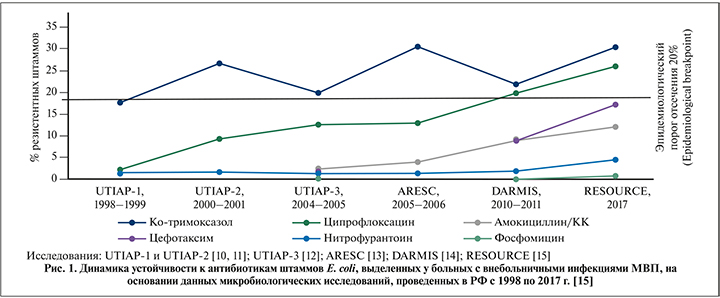
В исследовании RESOURCE [15] приведена динамика формирования устойчивости уропатогенной E. coli к антибиотикам в РФ (рис. 1). Следует обратить внимание на быстрое формирование устойчивости к фторхинолонам (за 20 лет увеличение с 2 до 26%), и, к сожалению, такая же тенденция прослеживается для амоксициллина/клавуланата и цефалоспоринов III поколения, что объясняет перевод этих антибиотиков в средства второй линии терапии. Минимальная устойчивость сохраняется только к нитрофуранам и фосфомицина трометамолу, хотя в отношении последнего есть определенная озабоченность в прогнозировании роста устойчивости, так как парентеральный фосфомицин за последние 5–7 лет стал широкого применяться в медицине для лечения инфекций, вызванных карбапенем-резистентной K. pneumoniae.
3. Экологическая безопасность антибактериальной терапии
Важность экологической безопасности применения антибиотиков впервые озвучивается в отечественных документах (Резолюция экспертного совета 2014 г. [1]) и Евразийских рекомендациях по рациональному применению антибиотиков в амбулаторной практике 2016 г. [2]. В этих документах указано на возможные экологически неблагоприятные последствия антибиотикотерапии, которые надо учитывать при создании рекомендаций по выбору антибиотиков для лечения различных инфекций наряду с природной антимикробной активностью и показателями антибиотикорезистентности.
Возможные экологически неблагоприятные последствия антибактериальной терапии приведены на рис. 2. Безопасность антибиотиков включает фармакологическую и экологическую безопасность. Как и все лекарственные препараты, антибиотики могут приводить к развитию нежелательных лекарственных реакций, которые включают аллергические реакции, идиосинкразию и органотоксичность. Аллергические реакции наиболее характерны для β-лактамных антибиотиков, чаще всего для природных и полусинтетических пенициллинов. Риск перекрестной аллергии на пенициллины и цефалоспорины невысок и для препаратов III поколения не превышает 1%. Органотоксичность – более актуальная нежелательная реакция, риск ее возникновения надо особенно учитывать в амбулаторной практике из-за сложности лабораторного контроля функции органов. Так, особую тревогу в последние годы вызывает органотоксичность фторхинолонов (нейротоксичность, кардиотоксичность, гепатотоксичность, артро- и хондротоксичность), что объясняет рекомендации регуляторных органов по ограничению назначения этих антибиотиков в амбулаторной практике при нетяжелых инфекциях, в частности для лечения цистита [18, 19].
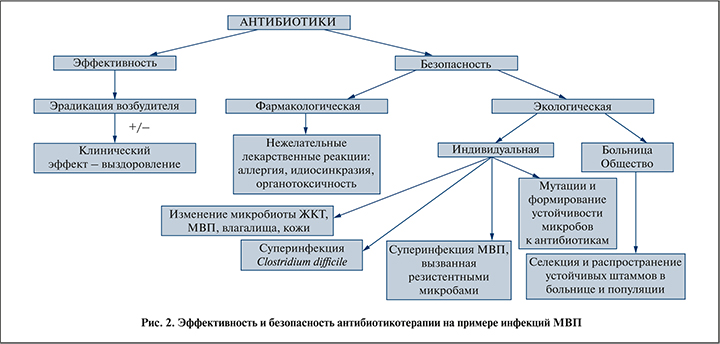
Экологически неблагоприятные последствия применения антибиотиков включают:
- изменение микробиоты желудочно-кишечного тракта, нижних МВП, влагалища, кожи;
- мутации микроорганизмов с формированием устойчивости к антибиотикам, селекция антибиотикорезистентных штаммов бактерий;
- развитие суперинфекции, вызванной Clostridium difficile (антибиотикассоциированная диарея и псевдомембранозный колит);
- развитие суперинфекции МВП, вызванной полирезистентными микроорганизмами.
Важным неблагоприятным экологическим последствием является изменение микробиома человека, прежде всего сбалансированной микробиоты кишечника, которое может сопровождаться не только формированием резистентности, но и существенными нарушениями обмена веществ в организме человека [20, 21]. Различные антибиотики в разной степени нарушают баланс кишечной микрофлоры и обусловливают риск формирования резистентных штаммов. К наиболее существенным и долго сохраняющимся изменениям микробиоты кишечника приводит применение фторхинолонов, клиндамицина и кларитромицина в сочетании с метронидазолом [22]. В то же время использование нитрофуранов не сопровождается выраженными изменениями микробиоты кишечника по сравнению с фторхинолонами [23, 24].
Влияние антибиотиков на кишечную микрофлору также связано с биодоступностью, т.е. степенью всасывания в кишечнике. Чем более полно всасывается антибиотик, тем меньше его остается в кишечнике и тем меньше будет повреждающее действие на микробиоту кишечника. По этой причине оптимизированные лекарственные формы антибиотика с более высокой биодоступностью в экологическом плане более безопасны. В частности, биодоступность растворимой калиевой соли фуразидина в комплексе с гидрокарбонатом магния (фурамаг, OlainFarm, Латвия) имеет биодоступность, более чем в 2 раза превышающую таковую при применении обычных таблеток фуразидина.
Повреждающее действие антибиотика на кишечную микрофлору и связанные с этим формирование и селекция антибиотикорезистентных штаммов принято обозначать коллатеральным повреждением (Collateral damage) или сопутствующим (параллельным) ущербом антибиотикотерапии. Антибиотики – таргентные препараты, способные распознавать свою уникальную мишень в прокариотической клетке. Любой антибиотик обладает определенным спектром антимикробной активности, т.е. имеет сродство к мишени, расположенной в разных микроорганизмах. При неосложненных инфекциях МВП основным целевым микробом является E. coli, в которой имеется мишень для многих антибиотиков. В результате подавление антибиотиком кишечной палочки при инфекции МВП является его терапевтическим действием, а подавление жизнедеятельности других микробов – нормальной микрофлоры кишечника, урогенитального тракта, кожи – рикошетом или сопутствующим ущербом. Для некоторых антибиотиков сопутствующий ущерб при его применении может превышать терапевтический, что приводит к серьезным нарушениям микробиоценоза или экологическим повреждениям. В идеале антибиотик должен иметь спектр действия не широкий, а достаточный для киллинга наиболее актуальных возбудителей инфекции. Таким образом, в амбулаторной практике при выборе антибиотика для лечения нетяжелых инфекций должен доминировать принцип «минимальной достаточности» спектра антимикробной активности, т.е. при прочих равных условиях надо отдавать предпочтение антибиотику с более узким спектром, что впервые обосновано в клинических рекомендациях по правилам применения антимикробных препаратов [2].
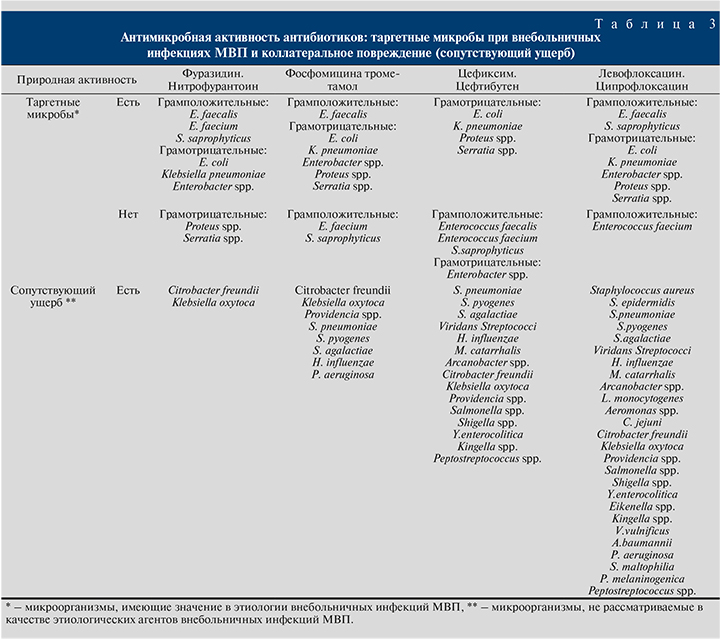
В табл. 3, в которой представлен природный спектр антибиотиков для лечения инфекций МВП, наглядно видно, что нитрофураны характеризуются минимальным сопутствующим ущербом при лечении цистита, а значит, должны быть предпочтительными антибиотиками в этой ситуации. В клинических рекомендациях IDSA и ESCMID применение нитрофуранов и фосфомицина в первой линии терапии цистита обосновывается именно их минимальным сопутствующим ущербом [7].

Некоторые антибиотики в большей, чем другие, степени способны провоцировать формирование устойчивости микроорганизмов и вызывать селекцию резистентных штаммов. Так, в работе M. Gobernado и et al. [25] показана прямая корреляционная зависимость между объемом потребления фторхинолонов в 20 больницах Испании и уровнем резистентности E. coli к фторхинолонам с коэффициентом корреляции 0,5 (p=0,025). Наибольший коллатеральный ущерб в амбулаторной практике наблюдается при применении цефалоспоринов III поколения, вызывающих селекцию β-лактамаз расширенного спектра и устойчивость к цефалоспоринам [26–29], фторхинолонов (селекция устойчивых стафилококков, синегнойной палочки, риск суперинфекции, вызванной C. difficile) [26, 27], азитромицина (рост устойчивости пневмококков и стрептококков к макролидам и β-лактамам) [30–32].
Классическим примером возникновения и селекции устойчивых микробов является широкое и необоснованное назначение ванкомицина внутрь для профилактики клостридиальной диареи в ОРИТ США в 1980-х гг. и быстрое распространение в этих отделениях ванкомицин-резистентных энтерококков [33].
В качестве разумных мер достижения экологической безопасности антимикробной терапии и минимизации риска сопутствующего (параллельного) ущерба в урологии можно предложить следующие мероприятия:
1. Ограничение необоснованного и пролонгированного применения антибиотиков для лечения и профилактики инфекций:
a. Не лечить бессимптомную бактериурию, за исключением беременных женщин;
b. Не лечить катетер-ассоциированную бактериурию и лейкоцитурию в отсутствие симптомов инфекции МВП;
c. Использовать короткие курсы периоперационной антибиотикопрофилактики – в идеале одна предоперационная доза, при высоком риске осложнений продление профилактики – максимум на 24 ч;
d. Исключить профилактические курсы антибиотиков при хронических и рецидивирующих инфекциях МВП. При необходимости профилактики использовать неантибактериальные средства (лиофилизированный лизат штаммов E. coli, D-манноза, клюква, фитопрепараты, вагинальная эстрогенозаместительная терапия в постменопаузе);
e. Не использовать продленные курсы антибиотиков при цистите: нитрофураны, β-лактамы >7 дней.
2. При выборе антибиотика отдавать предпочтение препаратам с низким потенциалом селекции устойчивых микроорганизмов и минимальным риском развития сопутствующего ущерба. В качестве средств первой линии терапии при неосложненном цистите обоснованно рекомендованы нитрофураны (фуразидин, нитрофурантоин) и фосфомицина трометамол не только из-за низкого уровня к ним резистентности, но и из-за минимального риска возникновения сопутствующего ущерба. При осложненном и рецидивирующем цистите более предпочтительными антибиотиками являются нитрофураны, так как, в отличие от фосфомицина, проявляют активность в отношении энтерококков и обладают более высоким эрадикационным потенциалом, что документировано в клинических исследованиях [34, 35].
Эксперты ВОЗ также обращают внимание врачей на принцип минимальной достаточности при назначении антибиотика для снижения риска сопутствующего ущерба.
В последнем документе ВОЗ приводятся три группы антибиотиков по приоритету выбора: ACCESS (приоритетный выбор – минимальный сопутствующий ущерб), WATCH (вторая линия, возможен сопутствующий ущерб), RESERVE (резерв в отсутствие другой альтернативы лечения) [36, 37]. Из антибиотиков для лечения инфекций МВП в группу приоритетного выбора ACCESS эксперты включили только нитрофурантоин, а фосфомицина трометамол, цефалоспорины III поколения и фторхинолоны приводятся в группе WATCH.
В заключение следует подчеркнуть, что экологическая безопасность антимикробной терапии служит важным компонентом сдерживания антибиотикорезистентности на глобальном и локальном уровнях.



